What Is Limb Salvage Surgery?
 Limb salvage surgery is a surgical procedure designed to prevent amputation of a limb. The main goal of this surgery is to save the limb, restore or improve its function, and help the patient return to their daily activities. Certain conditions may endanger your lower extremities and require surgery to prevent amputation of the affected limb. Specific types of bone fractures, advanced diabetic wounds, infections, cancers, frostbite, and poor circulation may need surgical intervention to save the affected limb. For more information about limb salvage surgery as it pertains to the lower extremities, please consult with a podiatrist.
Limb salvage surgery is a surgical procedure designed to prevent amputation of a limb. The main goal of this surgery is to save the limb, restore or improve its function, and help the patient return to their daily activities. Certain conditions may endanger your lower extremities and require surgery to prevent amputation of the affected limb. Specific types of bone fractures, advanced diabetic wounds, infections, cancers, frostbite, and poor circulation may need surgical intervention to save the affected limb. For more information about limb salvage surgery as it pertains to the lower extremities, please consult with a podiatrist.
Limb salvage can be an effective way in preventing the need for limb amputation. If you have diabetes, cancer, or any other condition that could lead to foot amputation if left unchecked, consult with Dr. Mark Gagnon from Advanced Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Limb Salvage?
Limb salvage is the attempt of saving a limb, such as the foot from amputation. Podiatrists also try to make sure that there is enough function in the foot after the salvage that it is still usable. Diabetes is the number one cause of non-traumatic amputations in the United States. Those with diabetes experience poor blood circulation, which prevents proper healing of an ulcer. If the ulcer is left uncheck, it could become infected, which could result in the need for amputation.
However, there are other causes as well, such as cancer and traumatic injury. Links between higher mortality rates and amputation have been found. This translates into higher healthcare costs, and a reduced quality of life and mobility for amputees. Podiatrists have attempted to increase the prevalence of limb salvage in an attempt to solve these issues.
Diagnosis and Treatment
Limb salvage teams have grown in recent years that utilize a number of different treatments to save the infected limb. This includes podiatrists that specialize in wound care, rehabilitation, orthotics, and surgery. Through a combination of these methods, limb salvage has been found to be an effective treatment for infected limbs, and as an alternative to amputation. Podiatrists will first evaluate the potential for limb salvage and determine if the limb can be saved or must be amputated.
If you have any questions, please feel free to contact one of our offices located in Crestwood, Orland Park, and Summit, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Limb Salvage
Limb salvage is a procedure that involves saving a lower extremity from amputation. In podiatry, limb amputation often occurs as a result of diabetes, peripheral vascular disease, neuropathy, cancer, and severe crush injury. The fundamental goal of limb salvage is to restore and maintain stability and movement of the affected lower extremity.
The procedure typically involves removing the diseased tissue and a small portion of the surrounding healthy tissue, as well as the removal of any affected bone if necessary. If the bone is removed, it is then replaced with prostheses, synthetic metal rods or plates, or grafts from either the patient’s body or a donor. Limb salvage is typically the preferred choice of procedure over amputation, as the procedure preserves both the patient’s appearance and allows for the greatest possible degree of function in the affected limb.
Upon diagnosis and determining that limb salvage is the appropriate treatment, the podiatrist may enlist the help of a physical and/or occupational therapist to prepare the patient for surgery by introducing various muscle-strengthening, walking, and range of motion exercises. Such exercises may be continued as rehabilitation post-procedure.
What Happens When a Stress Fracture Occurs?
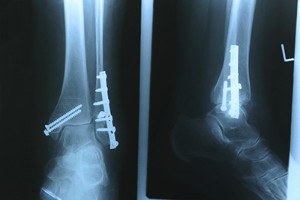 A stress fracture is a small hairline fracture that usually occurs because the foot is no longer able to handle the load being placed on it. While stress fractures can occur in the pelvis, thigh bones and shins, they most commonly occur in the lower legs, particularly in the bones of the midfoot. Because they often are a result of overuse and repetitive motion, as opposed to a specific injury, athletes such as runners, soccer players and dancers are at an increased risk for developing them. Stress fractures are often indicated by sharp pain when bearing weight, but as the fracture gets worse, the pain will persist even when not bearing weight. Those who are experiencing pain in their forefoot and believe that they may have a stress fracture should consult with a podiatrist for treatment.
A stress fracture is a small hairline fracture that usually occurs because the foot is no longer able to handle the load being placed on it. While stress fractures can occur in the pelvis, thigh bones and shins, they most commonly occur in the lower legs, particularly in the bones of the midfoot. Because they often are a result of overuse and repetitive motion, as opposed to a specific injury, athletes such as runners, soccer players and dancers are at an increased risk for developing them. Stress fractures are often indicated by sharp pain when bearing weight, but as the fracture gets worse, the pain will persist even when not bearing weight. Those who are experiencing pain in their forefoot and believe that they may have a stress fracture should consult with a podiatrist for treatment.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact Dr. Mark Gagnon from Advanced Podiatry. Our doctor can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Tennis or basketball players
- Gymnasts
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact one of our offices located in Crestwood, Orland Park, and Summit, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Stress Fractures of the Foot and Ankle
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.
What Are the Symptoms of a Broken Toe?
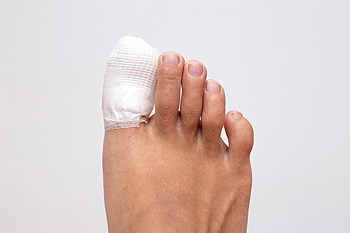 Patients who stub their toe against a piece of furniture, or drop a heavy object on it, may experience a broken toe. The average healing time for this type of injury is generally four to six weeks, and it is often accompanied by swelling and bruising. Additional symptoms can include severe pain and it may be difficult to put a shoe on and walk. Mild relief can be found if you have a mildly fractured toe by taping the affected toe to the toe next to it. This is referred to as buddy taping, and it is typically effective in providing the necessary stability to the affected toe as the healing process occurs. Severely broken toes may require that a cast be worn, and it can be helpful to use crutches to keep weight off of the toe. If you have fractured your toe, please consult with a podiatrist.
Patients who stub their toe against a piece of furniture, or drop a heavy object on it, may experience a broken toe. The average healing time for this type of injury is generally four to six weeks, and it is often accompanied by swelling and bruising. Additional symptoms can include severe pain and it may be difficult to put a shoe on and walk. Mild relief can be found if you have a mildly fractured toe by taping the affected toe to the toe next to it. This is referred to as buddy taping, and it is typically effective in providing the necessary stability to the affected toe as the healing process occurs. Severely broken toes may require that a cast be worn, and it can be helpful to use crutches to keep weight off of the toe. If you have fractured your toe, please consult with a podiatrist.
Broken toes may cause a lot of pain and should be treated as soon as possible. If you have any concerns about your feet, contact Dr. Mark Gagnon from Advanced Podiatry. Our doctor will treat your foot and ankle needs.
What Is a Broken Toe?
A broken toe occurs when one or more of the toe bones of the foot are broken after an injury. Injuries such as stubbing your toe or dropping a heavy object on it may cause a toe fracture.
Symptoms of a Broken Toe
- Swelling
- Pain (with/without wearing shoes)
- Stiffness
- Nail Injury
Although the injured toe should be monitored daily, it is especially important to have a podiatrist look at your toe if you have severe symptoms. Some of these symptoms include worsening or new pain that is not relieved with medication, sores, redness, or open wounds near the toe.
If you have any questions, please feel free to contact one of our offices located in Crestwood, Orland Park, and Summit, IL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
What to Know About a Broken Toe
Trauma to the foot, especially the toes, can occur in many ways. Banging them, stubbing them, or dropping something on them are a few different ways this trauma can occur. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break or fracture. Another type of trauma that can break a toe is repeated activity that places stress on the toe for prolonged periods of time.
Broken toes can be categorized as either minor or severe fractures. Symptoms of minor toe fractures include throbbing pain, swelling, bruising on the skin and toenail, and the inability to move the toe with ease. Severe toe fractures require medical attention and are indicated when the broken toe appears crooked or disfigured, when there is tingling or numbness in the toe, or when there is an open, bleeding wound present on the toe.
Generally, a minor toe break will heal without long-term complications. However, it is important to discontinue activities that put pressure on the toe. It is best to stay off of the injured toe and immediately get a splint or cast to prevent any more additional movement of the toe bones. You can also immobilize your toe by placing a small cotton ball between the injured toe and the toe beside it. Then, tape the two toes together with medical tape. Swelling can be alleviated by placing an ice pack on the broken toe directly as well as elevating your feet above your head.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery, especially when the big toe has been broken. Due to its position and the pressure the big toe endures with daily activity, future complications can occur if it is not properly treated. Pain associated with minor toe fractures can be managed with over-the-counter pain medications. Prescription pain killers may be necessary for severe toe fractures.
The healing time for a broken toe is approximately four to six weeks. In severe cases where the toe becomes infected or requires surgery, healing time can take up to eight weeks or more. While complications associated with a broken toe are immediately apparent, it is important to note that there are rare cases when additional complications, such as osteoarthritis, can develop over time. You should immediately speak with your podiatrist if you think you have broken your toe due to trauma. They will be able to diagnose the injury and recommend the appropriate treatment options.
Fat Pad Loss in Elderly Feet
 Elderly people may experience foot conditions as a result of standing and walking throughout their lifetime. Foot problems may occur due to a loss of fat in the foot. The fat pad in the foot generally provides adequate padding, and is responsible for shock absorption. Additionally, fractures may be more likely in elderly people, and their balance may be affected as the aging process occurs. A common condition among seniors is dry skin, and this can be remedied by applying a good moisturizer as part of the bedtime routine. Older people may see changes in their toenails, where they gradually become brittle, yellowed, and thicker. If you would like additional information about how to provide proper care for your elderly relative’s feet, please consult with a podiatrist.
Elderly people may experience foot conditions as a result of standing and walking throughout their lifetime. Foot problems may occur due to a loss of fat in the foot. The fat pad in the foot generally provides adequate padding, and is responsible for shock absorption. Additionally, fractures may be more likely in elderly people, and their balance may be affected as the aging process occurs. A common condition among seniors is dry skin, and this can be remedied by applying a good moisturizer as part of the bedtime routine. Older people may see changes in their toenails, where they gradually become brittle, yellowed, and thicker. If you would like additional information about how to provide proper care for your elderly relative’s feet, please consult with a podiatrist.
Proper foot care is something many older adults forget to consider. If you have any concerns about your feet and ankles, contact Dr. Mark Gagnon from Advanced Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
The Elderly and Their Feet
As we age we start to notice many changes in our body, but the elder population may not notice them right away. Medical conditions may prevent the elderly to take notice of their foot health right away. Poor vision is a lead contributor to not taking action for the elderly.
Common Conditions
- Neuropathy – can reduce feeling in the feet and can hide many life-threatening medical conditions.
- Reduced flexibility – prevents the ability of proper toenail trimming, and foot cleaning. If left untreated, it may lead to further medical issues.
- Foot sores – amongst the older population can be serious before they are discovered. Some of the problematic conditions they may face are:
- Gouging toenails affecting nearby toe
- Shoes that don’t fit properly
- Pressure sores
- Loss of circulation in legs & feet
- Edema & swelling of feet and ankles
Susceptible Infections
Diabetes and poor circulation can cause general loss of sensitivity over the years, turning a simple cut into a serious issue.
If you have any questions please feel free to contact one of our offices located in Crestwood, Orland Park, and Summit, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Taking Care of Elderly Feet
Many foot diseases and conditions become more serious and common among the elderly. Some of these conditions include diabetic ulcers, ingrown toenails, fungus, arthritis, corns, and calluses. Unfortunately, it may be harder for older adults to take care of their own feet, but there are some precautions they can take in order to avoid any serious conditions.
Dry, cracked heels tend to be a common problem for older people. In order to avoid this, you should always keep your feet clean and well moisturized. Special feet moisturizers should be used as average lotions might not provide enough moisture for dry and cracked heels. Daily foot inspections are crucial for the elderly to detect any irregularities in their earliest stages. During the aging process, blood circulation tends to slow down causing older people to not feel their feet as well as they used to. This often results in foot problems going unnoticed.
Fungal and bacterial conditions thrive on elderly feet because older adults are less likely to keep their feet clean and dry; this makes it easier for bacteria to take hold in their dry, cracked skin. Elderly people should be sure to thoroughly dry their feet, especially in between the toes, after bathing. This will help them avoid developing any fungal infections. Additionally, clean cotton socks should be worn after the feet are dried.
Cutting toenails straight across will help prevent ingrown toenails. When toenails are cut too lose, the nail might break through the skin resulting in an ingrown nail. Clippers should be used to cut the nails in order to make the cut even.
Elderly people who have diabetes are at risk of developing serious foot problems that may lead to amputation. Ulcers that are left untreated can lead to gangrene. Dry and cracked feet, fungus, and untended cuts under the nails may also lead to infections.
Fortunately, Medicare covers many different types of services for foot care. Elderly people with any of these foot conditions should seek the help of a podiatrist and perform daily foot inspections in order to ensure that they have healthy feet.
What Type of Corn Do I Have?
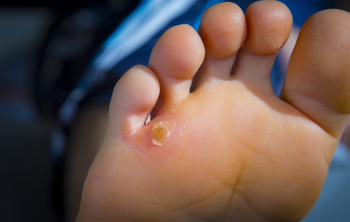 Excessive friction is generally the reason why a corn on the foot can develop. This can happen for a variety of reasons, including wearing shoes that do not fit correctly, running consistently, or possibly from abnormal bone structure. A common place for a corn to develop is on the pinky toe. As small as the corn may be, it is able to cause severe pain and discomfort, and wearing shoes can become difficult. Some patients have a corn that develops between the toes. These are considered to be soft corns, and will stay moist as a result of wearing socks for the majority of the day. Mild relief may be found when the corn is covered by a protective pad, and it may help to wear larger size shoes. If you have any type of corn on your foot, please consult with a podiatrist who can offer the best treatment options for you.
Excessive friction is generally the reason why a corn on the foot can develop. This can happen for a variety of reasons, including wearing shoes that do not fit correctly, running consistently, or possibly from abnormal bone structure. A common place for a corn to develop is on the pinky toe. As small as the corn may be, it is able to cause severe pain and discomfort, and wearing shoes can become difficult. Some patients have a corn that develops between the toes. These are considered to be soft corns, and will stay moist as a result of wearing socks for the majority of the day. Mild relief may be found when the corn is covered by a protective pad, and it may help to wear larger size shoes. If you have any type of corn on your foot, please consult with a podiatrist who can offer the best treatment options for you.
If you have any concerns regarding your feet and ankles, contact Dr. Mark Gagnon of Advanced Podiatry. Our doctor will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
- Well-fitting socks
- Comfortable shoes that are not tight around your foot
- Shoes that offer support
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctor to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact one of our offices located in Crestwood, Orland Park, and Summit, IL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.